Lung cancer continues to be the most significant oncological challenge in the United States. It has remained the leading cause of cancer death among men since the early 1950s and among women since 1987. Globally, it has held the position of the deadliest cancer for several decades. While low dose computed tomography (LDCT) has proven to be a powerful tool in reducing mortality, new data suggests that current implementation and restrictive eligibility criteria are leaving thousands of lives at risk.
The Proven Efficacy of LDCT Screening
The effectiveness of LDCT screening is well established through two large scale randomized clinical trials. These studies demonstrated that regular screening with LDCT significantly reduces lung cancer mortality. Currently, approximately 13 million high risk adults in the U.S. are recommended for this screening, representing a massive opportunity to combat the nation’s deadliest cancer.
Despite this evidence, the transition from clinical trials to public health success has been difficult. More than 80 percent of adults who are currently eligible for screening do not actually receive it.
The Impact of Low Screening Uptake
A recent analysis published in JAMA highlights the stark reality of current screening rates. Researchers found that in 2024, only 18.7 percent of eligible adults reported undergoing lung cancer screening. This level of participation is described by experts as unacceptably low.
Even at this low level of uptake, the public health benefits are measurable:
- Screening prevents nearly 15,000 lung cancer deaths over a five year period.
- More than 190,000 life-years are saved within that same five year window.
However, the potential for improvement is vast. If screening reached 100 percent of the currently eligible population, the number of deaths prevented would increase by more than 300 percent. This would result in an estimated 62,000 prevented deaths and more than 870,000 life-years gained over five years. Notably, these gains in life-years from full screening uptake are substantially greater than the estimated gains from therapeutic advances for patients with late-stage disease.
Addressing Restrictive Eligibility Criteria
Beyond the issue of uptake, researchers are concerned that current eligibility criteria are overly restrictive. Evidence suggests that current guidelines exclude approximately 50 percent of adults who are eventually diagnosed with lung cancer.
The analysis identified nearly 30,000 potentially preventable deaths over five years among adults with a smoking history who did not qualify under the 2021 U.S. Preventive Services Task Force (USPSTF) criteria. These deaths occurred in specific high risk groups:
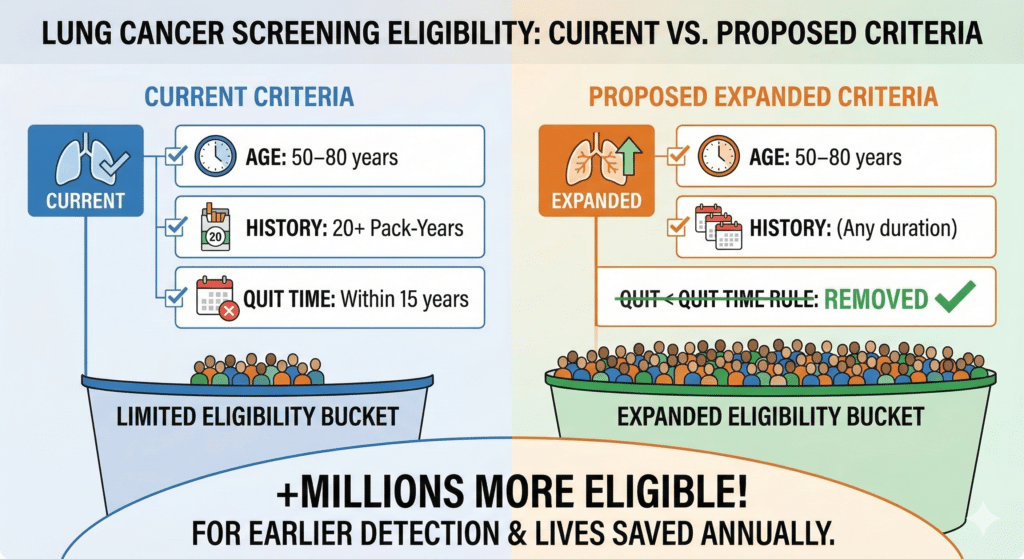
- 36 percent of these deaths were among adults with at least 20 pack-years of smoking who had quit more than 15 years prior.
- Another 36 percent were among adults who currently smoke or quit within the last 15 years and have at least 20 years of smoking history, but fall below the 20 pack-year threshold.
In response to these findings, the National Comprehensive Cancer Network and the American Cancer Society have already removed the requirement that a person must have quit within the last 15 years. Additionally, shifting to a 20 year smoking duration criterion rather than the complex pack-year calculation could expand eligibility to more high risk individuals with minimal loss in screening efficiency.
Broadening the Scope of Early Detection
While smoking history remains a primary risk factor, lung cancer also affects those who have never smoked. Approximately 20,000 individuals who have never smoked die of lung cancer in the U.S. every year. Furthermore, nearly 4,700 cases are diagnosed annually in adults younger than 50, a group generally excluded from current age based criteria.
Expanding recommendations to these populations typically requires high quality randomized trial data, which is often considered prohibitively expensive. However, advances in technology offer new solutions. Deep learning algorithms like Sybil can predict future lung cancer risk from a single LDCT scan. These tools may allow for better risk stratification and provide opportunities to study screening in high risk individuals regardless of their tobacco history.
A Call for National Action
The data is clear: increasing the uptake of lung cancer screening must be a leading public health priority. Achieving the full potential of this technology requires a three-pronged approach:
- Increasing uptake among currently eligible adults.
- Thoughtfully expanding eligibility criteria to include more high risk individuals.
- Harnessing technological advances in risk prediction to reach all high risk populations, including those without a tobacco history.
Lung cancer screening has already saved tens of thousands of lives in the decade since its implementation. To save tens of thousands more, the medical community must move to ensure these tools are reaching every person at risk.