For decades, the medical community has recognized a link between carrying excess weight and various health complications. However, as we move through 2026, the data has become undeniable: obesity is not just a metabolic hurdle; it is a primary driver of the global cancer epidemic. At UDS Health, we believe that understanding the biological “why” behind this connection is essential for both prevention and treatment.
A landmark translational science review published in JAMA has laid out the most comprehensive map to date of how excess adiposity—body fat—alters human biology to create a fertile ground for malignancies. This article distills that complex big data into a clear, long-form editorial on the state of obesity-driven oncology in 2026.
You can access the full JAMA translational science review here.
The Scale of the Crisis
By 2026, the statistics surrounding obesity have reached a critical mass. Globally, more than 1 billion people are now living with obesity. In the United States, the figures are even more stark, with nearly 42% of adults classified as having obesity.
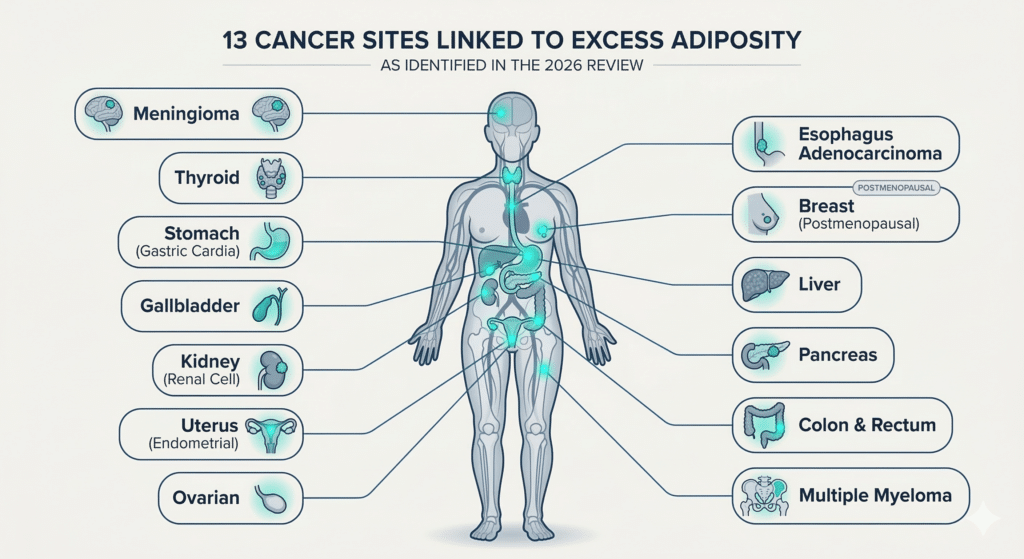
This is no longer just a “lifestyle” issue. The data now confirms that obesity is associated with an increased risk of at least 13 different types of cancer. These include some of the most common and most deadly forms of the disease:
- Postmenopausal breast cancer
- Colorectal cancer
- Endometrial (uterine) cancer
- Esophageal adenocarcinoma
- Pancreatic, kidney, and liver cancers
The Biological Connection: Why Fat Drives Cancer
One of the most significant contributions of the 2026 JAMA review is the detailed breakdown of the biological mechanisms that turn excess fat into a pro-cancer environment. Adipose tissue is not an inert storage depot; it is an active endocrine organ that communicates with the entire body.
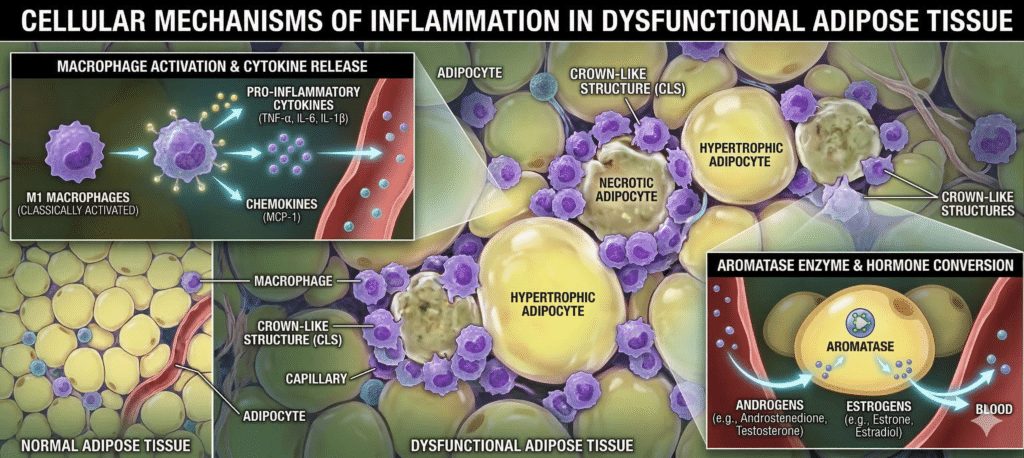
1. Chronic Low-Grade Inflammation
Obesity triggers a state of constant, low-level inflammation throughout the body. As fat cells (adipocytes) grow too large, they can become oxygen-deprived and die, attracting immune cells like macrophages. These macrophages form “crown-like structures” around dead fat cells, secreting inflammatory chemicals that damage DNA and encourage cells to grow uncontrollably.
2. Insulin and Growth Factors
Excess body fat often leads to insulin resistance, causing the pancreas to produce more insulin. High levels of insulin, along with a related protein called Insulin-like Growth Factor-1 (IGF-1), act like “fertilizer” for cancer cells, telling them to divide rapidly and ignore the body’s natural signals to die.
3. Sex Hormone Imbalance
For many, the most direct link to cancer is through hormones. Adipose tissue contains an enzyme called aromatase, which converts other hormones into estrogen. In postmenopausal individuals, excess fat becomes the primary source of estrogen, significantly increasing the risk of estrogen-driven cancers like breast and endometrial cancer.
The Role of the Microbiome
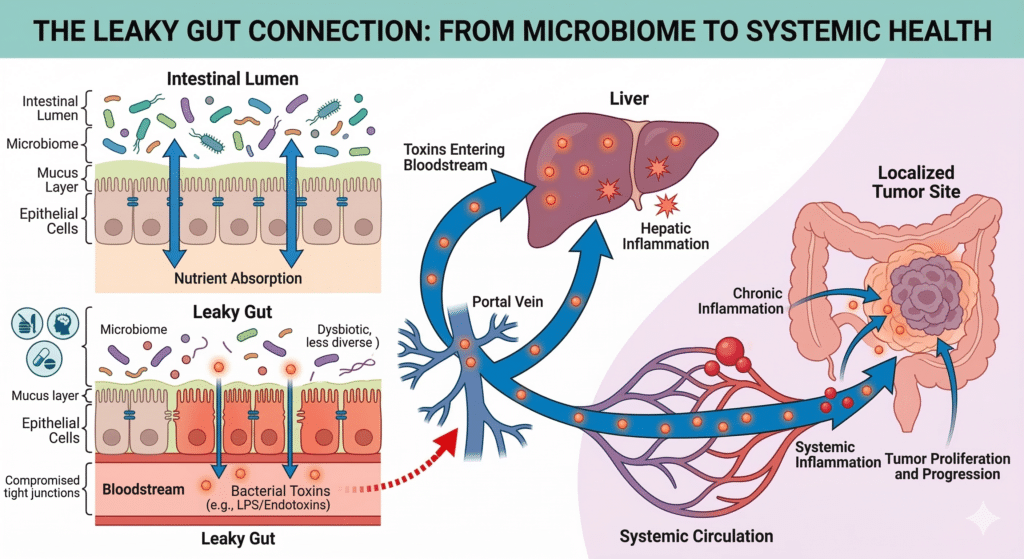
In 2026, we are also gaining a deeper understanding of the “gut-lung-heart-cancer” axis. Obesity significantly alters the gut microbiome—the trillions of bacteria living in our intestines.
An “obese” microbiome can lead to a “leaky gut,” allowing bacterial toxins to enter the bloodstream. These toxins further fuel the systemic inflammation that drives cancer progression, particularly in the liver and colon.
Treatment Breakthroughs: GLP-1s and Bariatric Surgery
While the data on risk is sobering, the 2026 report also highlights powerful tools for risk reduction. We are entering a new era where intentional weight loss is being proven to lower cancer incidence.
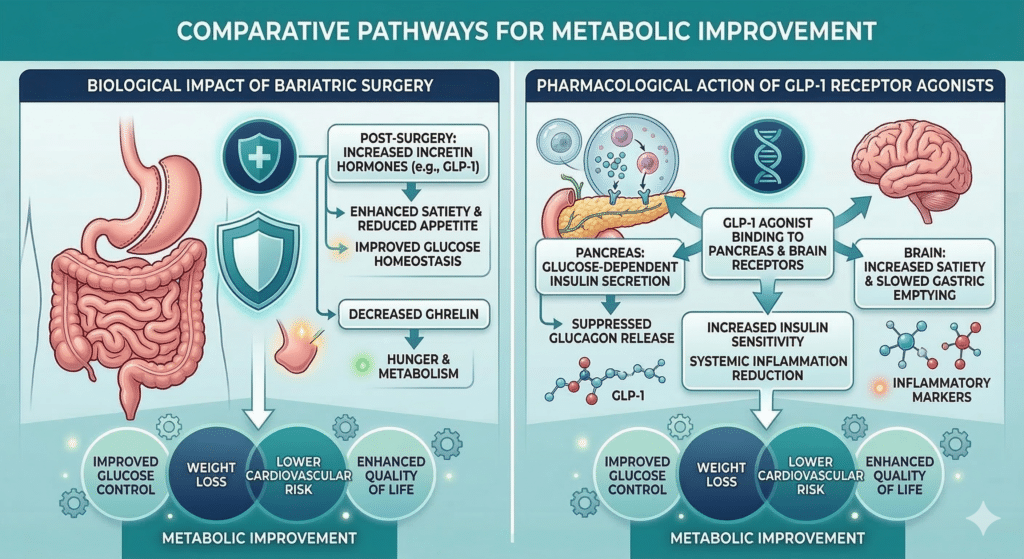
The Impact of Bariatric Surgery
Long-term studies now show that individuals who undergo bariatric surgery have a significantly lower risk of developing obesity-related cancers compared to those who do not. The risk reduction is most pronounced in women, particularly for breast and endometrial cancers.
The GLP-1 Revolution
The rise of GLP-1 receptor agonists (like semaglutide and tirzepatide) has changed the conversation in 2026. While these drugs were originally for diabetes and weight loss, emerging data suggests they may also reduce cancer risk by improving insulin sensitivity and reducing systemic inflammation.
Closing the Disparity Gap
As Chief Editor, I must highlight that the burden of obesity-driven cancer is not shared equally. Disparities in access to healthy food, safe places for physical activity, and advanced medical treatments mean that marginalized communities are often hit the hardest. Addressing these social determinants of health is a cornerstone of the 2026 public health strategy.
A Vision for the Future
The 2026 JAMA review makes one thing clear: we cannot treat cancer in a vacuum. To win the fight against cancer, we must also win the fight against the biological triggers caused by obesity. This means moving beyond “eat less, move more” and toward precision medicine that addresses inflammation, hormone balance, and metabolic health.
At UDS Health, we remain committed to translating this translational science into clinical action. The more we understand the heavy toll of obesity, the better we can protect the health of our patients.